In an age where medical science is making remarkable strides in fertility and reproduction, in vitro fertilisation (IVF) has emerged as one of the most widely-used assisted reproductive technologies (ART) for couples facing fertility challenges. Whether due to blocked fallopian tubes, low sperm count, or unexplained infertility, IVF offers hope by enabling fertilisation of an egg outside the body, followed by embryo transfer into the uterus. In this article, we’ll explore how IVF works, why it is used, the step-by-step process, key success-factors, risks, ethical considerations, and what couples in India and elsewhere should know before proceeding.
What is IVF?
In simple terms, IVF is a method in which mature eggs are retrieved from the woman’s ovaries and fertilised with sperm in a laboratory (“in vitro” means “in glass”). The resulting embryos are then transferred into the uterus with the aim of achieving pregnancy.
Unlike natural conception — where the egg and sperm meet inside the fallopian tube — IVF bypasses the fallopian tubes altogether and brings fertilisation into a controlled lab environment.
The idea is to increase the odds of fertilisation, embryo development and successful implantation by controlling many of the variables outside the body.
Why IVF is used: Indications and benefits
There are several reasons couples might opt for IVF:
- Blockage or damage of fallopian tubes, which obstruct the egg-sperm meeting in natural conception.
- Severe male-factor infertility (e.g., low sperm count or motility).
- Endometriosis, ovulatory dysfunction, diminished ovarian reserve, unexplained infertility.
- Genetic disorders: IVF allows for preimplantation genetic testing (PGT) so that embryos can be checked for specific chromosomal or gene-based conditions before transfer.
- Fertility preservation (e.g., for cancer patients) where eggs or embryos are frozen ahead of treatment. Mayo Clinic
In short, IVF is often the “go-to” treatment when simpler fertility treatments (ovulation induction, intrauterine insemination) have failed or are unlikely to succeed.
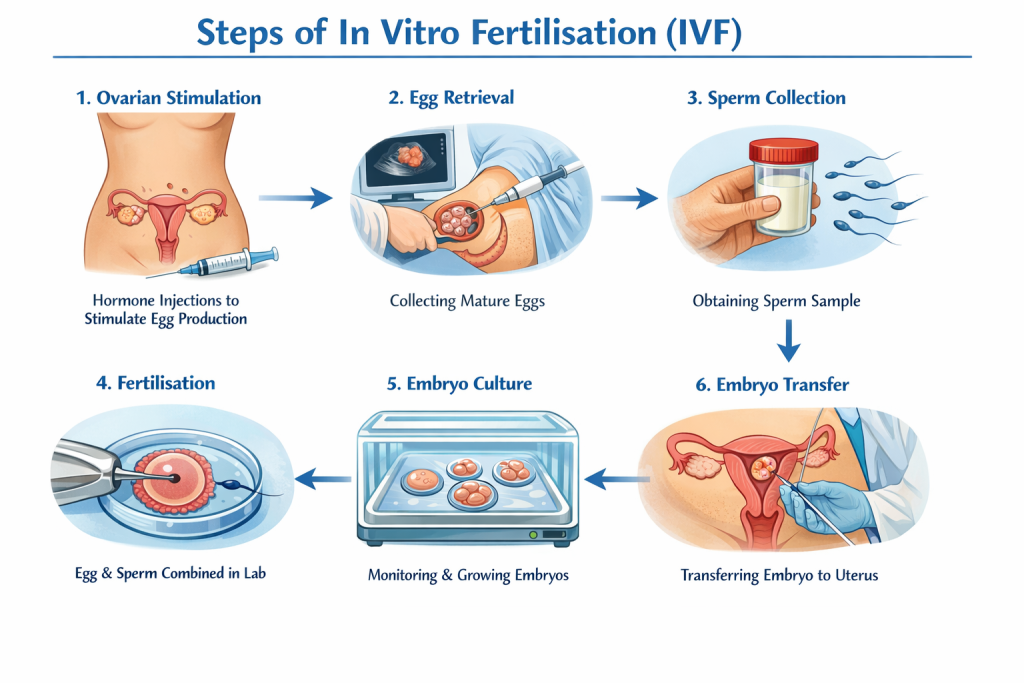
Step-by-Step: How the In Vitro Fertilisation Process Works
Here is a breakdown of the typical IVF cycle, illustrating each major step and what patients can expect.
1. Ovarian stimulation
The first phase involves administering hormonal medications (e.g., follicle-stimulating hormone [FSH], luteinizing hormone [LH] analogues) to stimulate the woman’s ovaries to produce multiple mature eggs — rather than the single egg that would normally develop in a menstrual cycle.
This is important because not every egg will fertilise or develop into a viable embryo — having multiple eggs increases the chances of success.
The clinic monitors the growing follicles with blood tests and ultrasound until the eggs reach appropriate maturity.
2. Egg retrieval (oocyte retrieval)
When the eggs are deemed mature, a trigger shot (often human chorionic gonadotropin, hCG) is given and after about 36 hours a minor surgical procedure is performed to retrieve the eggs. The retrieval is done under mild sedation, guided by ultrasound: a thin needle is inserted through the vaginal wall into the ovarian follicles to collect the eggs.
This step typically takes about 20-30 minutes, and the woman may experience mild cramping afterwards.
3. Sperm collection and preparation
On the same day as egg retrieval, the male partner provides a semen sample (or donor sperm is used). The sperm are processed in the lab to select the healthiest, motile sperm. In some cases, for severe male-factor infertility, a technique called intracytoplasmic sperm injection (ICSI) may be used, where a single sperm is injected directly into the egg.
4. Fertilisation and embryo culture
In the lab, the mature eggs are exposed to sperm in a culture medium (classic insemination) or via ICSI. After fertilisation is confirmed (usually the next morning), the embryos are cultured for several days—commonly up to 5 or 6 days (blastocyst stage) to assess their development.
During culture the embryologist monitors growth, cell division, embryo quality and may perform assisted hatching or other adjunctive techniques if required.
5. Embryo transfer
One or more selected embryos are transferred into the woman’s uterus via a thin catheter inserted through the cervix. This is typically done 3–6 days after fertilisation. The number of embryos transferred depends on the woman’s age, embryo quality, and clinic guidelines (to minimise multiple pregnancies).
After transfer, patients may continue hormone support (for example progesterone) to encourage implantation.
6. Pregnancy test and follow-up
Approximately 10–14 days after egg retrieval, a blood test is carried out to detect the pregnancy hormone (hCG) to determine whether implantation has occurred. If positive, prenatal care continues; if negative, options include frozen embryo transfer or another fresh cycle.
Success Factors and What Influences IVF Outcomes
The success of an IVF cycle depends on many inter-linked factors:
- Maternal age: Younger women have better egg quality and higher success rates. As age advances, chances decline.
- Egg and embryo quality: The number of mature eggs retrieved, how many fertilise, how many develop into top-grade embryos, all matter.
- Cause of infertility: Underlying reasons like diminished ovarian reserve or severe male-factor infertility may influence outcomes.
- Clinic protocols and lab conditions: The performance of the embryology laboratory, culture conditions, timing of transfer and selection of embryos are crucial.
- Lifestyle and health of both partners: Factors such as BMI, smoking, chronic diseases, and uterine health can affect implantation and pregnancy.
- Individualised treatment: Tailoring stimulation protocols, monitoring closely, adjusting medication doses increases odds of success.
It’s worth noting that while successes are encouraging, not every cycle works the first time — many couples may need multiple cycles.
Risks and Potential Complications of In Vitro Fertilisation
As with any medical procedure, IVF carries some risks and potential complications. It’s important for couples to be aware of these:
- Ovarian hyperstimulation syndrome (OHSS): When the ovaries respond too strongly to stimulation, causing swelling, pain, nausea, or in severe cases, serious complications.
- Multiple pregnancies: Transferring multiple embryos increases risk of twins, triplets, which are associated with higher risks for preterm birth, low birth weight, pregnancy complications.
- Ectopic pregnancy: While rare, a fertilised embryo may implant outside the uterus (e.g., in a fallopian tube).
- Bleeding/infection: During egg retrieval, minor bleeding or infection may occur.
- Emotional and financial stress: IVF can be emotionally challenging and expensive; couples must prepare for possibilities of unsuccessful cycles.
- Future child risks: Some studies indicate a slightly elevated risk of certain birth defects or low birth weight in IVF‐conceived babies, though maternal age remains the primary risk factor.
Despite these risks, for many couples the benefits outweigh the downsides when guided by experienced fertility specialists.
Ethical, Legal and Social Considerations
IVF raises several ethical and social issues that merit careful thought:
- Embryo freezing and disposal: When more embryos are created than transferred, decisions must be made about storage, donation, or disposal.
- Donor gametes and surrogacy: Use of donor eggs/sperm or gestational carriers introduces questions of genetic parenthood, rights, and regulation.
- Preimplantation genetic testing (PGT): While PGT can reduce risk of inherited disease, ethical lines around “designer babies” or selecting traits must be navigated.
- Access and equity: IVF can be costly and not accessible for all. In some countries legal and regulatory frameworks vary widely.
- Emotional well-being: Couples may face uncertainty, repeated cycles, grief of failure — psychological counselling is often beneficial.
IVF in India: What Couples Should Know
Many fertility clinics now offer IVF with donor eggs, sperm, or embryo banking; yet clarity about costs, success rates, and transparent communication is essential.
- Couples should ask about the clinic’s live birth rate (not just pregnancy rate), lab accreditation, number of cycles performed, and embryo handling policies.
- Costs can vary significantly—stimulations, medications, laboratory culture, embryo freezing, transfer — so budget planning is critical.
- Legal aspects: India’s Assisted Reproductive Technology (ART) Regulation Bill (pending/varied state-level) aims to standardise protocols; couples should check state-licensing and clinic certification.
- Lifestyle optimisation: In the Indian context, addressing obesity, PCOS, diabetic control, male lifestyle factors (smoking, alcohol, heat exposure) has added value.
Tips for Improving IVF Success
Here are practical tips to increase the chance of a successful outcome:
- Choose the right clinic: Investigate the clinic’s lab facilities, embryologist expertise, success statistics, and patient support services.
- Prepare your health: Maintain a healthy body mass index (BMI), control any medical conditions like diabetes or thyroid, avoid smoking and excessive alcohol, and consider mild exercise.
- Understand your protocol: Ask your doctor about the stimulation protocol, number of eggs expected, embryo culture duration.
- Manage stress and expectations: Emotional support or counselling helps you cope with the ups and downs of treatment.
- Lifestyle optimisation for male partner: Sperm quality matters — good nutrition, avoiding high-heat environments (e.g., hot tubs), limiting smoking/alcohol help.
- Consider embryo quality and timing: Ask whether embryos will be cultured to blastocyst stage (day 5/6) for better selection, ask about freezing policy for good extra embryos.
- Budget realistically: Many couples may need more than one cycle — plan finances accordingly rather than expecting success in the first attempt.
Future Trends in In Vitro Fertilisation
The field of IVF continues to evolve with new technologies and innovations:
- Time-lapse embryo monitoring and AI-based embryo selection are emerging to improve implantation prediction. arXiv+1
- Freeze-all strategies (retrieval and freezing all embryos then transferring later) are gaining popularity to improve outcomes and reduce OHSS risk.
- Genetic and epigenetic screening are being refined to increase safety and reduce risk of inherited disease.
- Research into in vitro gametogenesis (creation of gametes from stem cells) may one-day open new frontiers in fertility.
- Personalised medicine: Tailoring stimulation and embryo transfer protocols based on individual genetics, ovarian reserve, sperm DNA fragmentation.
As these advances become more mainstream, ethical and regulatory frameworks will need to keep pace.
Conclusion
In vitro fertilisation (IVF) offers a powerful pathway for many couples to achieve parenthood when natural conception proves difficult. By understanding the full process — from ovarian stimulation through embryo transfer, the factors influencing success, associated risks, and the ethical landscape — prospective parents can approach IVF with realistic expectations and informed decisions. For Indian couples in Chennai or elsewhere, choosing a reputable centre, optimising health, and preparing emotionally and financially are key steps. IVF may not guarantee pregnancy in one cycle, but with the right support, it significantly enhances the chance of building a family.
References
- “In vitro fertilization (IVF) – Mayo Clinic” – Mayo Clinic. Mayo Clinic
- “In Vitro fertilisation – What is it and what is it?” – Invimed. invimed.pl
- “Assisted Reproductive Technologies Meaning, Types and Causes” – Aakash. Aakash Educational Services
- “In vitro fertilisation treatment and factors affecting success” – PubMed article. PubMed
- “In Vitro Fertilization (IVF) Treatment & Process | Cleveland Clinic.” Cleveland Clinic
- “IVF (In Vitro Fertilization): Procedure & How It Works.” – Cleveland Clinic. Cleveland Clinic
- “Intracytoplasmic sperm injection” – Wikipedia. Wikipedia
- “Robust and generalizable embryo selection based on artificial intelligence and time-lapse image sequences.” – arXiv. arXiv
- “Data-Driven Prediction of Embryo Implantation Probability Using IVF Time-lapse Imaging.” – arXiv. arXiv